by mandy | Jul 3, 2024 | Detox, Evidence Based, Nutrients, Science-Based, Wellness
The Hidden Impact of Copper Toxicity and Histamine Intolerance Copper toxicity is a lesser-known yet significant factor that can lead to various health issues, including histamine intolerance. Histamine, an essential compound in the body, plays a vital role in immune responses, gastric acid secretion, and neurotransmission. However, when histamine levels are imbalanced, it can result [...]

by mandy | Apr 12, 2024 | Digestive/Urinary, Evidence Based, Science-Based, Success Stories
Patient Profile Name: Jane Doe Age: 43 Gender: Female Main Complaints: Frequent bladder infections characterized by burning, pain, and frequent urination. Diagnostic Findings Jane's condition was extensively evaluated using various diagnostic tools: Microgen Testing: Revealed a bacterial imbalance with low levels of Lactobacillus gasseri and the presence of E. coli, Streptococcus anginosus, Streptococcus oralis, and [...]

by mandy | Apr 8, 2024 | Detox, Digestive/Urinary, Evidence Based, Nutrients, Science-Based
Introduction Navigating the relentless cycle of recurrent urinary tract infections (UTIs) can be a source of significant frustration and discomfort for many. This persistent health challenge often leaves individuals seeking answers beyond conventional treatments, yearning for a lasting solution to their recurrent plight. The aim of this blog is to delve into the critical role [...]
by mandy | Mar 28, 2024 | Digestive/Urinary, Evidence Based, Inflammation, Nutrients, Wellness
Introduction LL-37, the only human cathelicidin antimicrobial peptide, emerges as a crucial player in our body's defense against infections. Originating from the CAMP (Cathelicidin Antimicrobial Peptide) gene, LL-37 is produced by various cells throughout the body, including epithelial cells and white blood cells. Its primary role lies in its potent antimicrobial activity, capable of destroying [...]

by mandy | Mar 24, 2024 | Detox, Diet, Digestive/Urinary, Evidence Based, Oxalate, Science-Based, Wellness
In a recent presentation, Dr. Aaron Miller of the Cleveland Clinic shared groundbreaking findings about oxalates, their interaction with the microbiome, and bile acids, drawing attention from Susan Owens and members who had the opportunity to engage in a Q&A session. I also did a video on the implications of oxalate and dysbiosis. Notably, Dr. [...]
by mandy | Mar 24, 2024 | Detox, Evidence Based, Genetics, Inflammation, Nutrients, Nutrition, Science-Based, Supplements
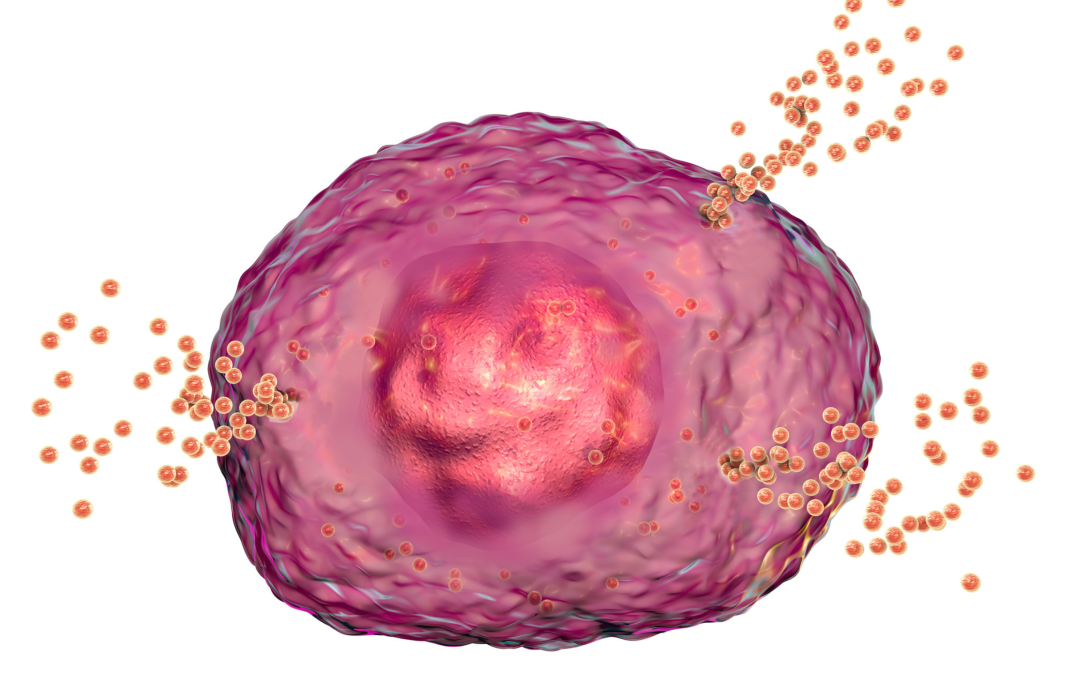
The intricate interactions within our body's immune system, particularly involving mast cells, play a crucial role in inflammation and allergic reactions. These cells, when triggered by external substances (antigens), can cause inflammation and produce various chemicals that lead to allergic symptoms. Central to this process is a protein called spleen tyrosine kinase (Syk), which, when [...]







